My new normal? Being that this is my temporary new normal, doesn’t make it much easier to handle, it also doesn’t make it normal at all. It just makes it my life. Most people don’t really know the extent of what it’s like unless they’ve experienced it as only they can through their body or they have lived with someone going through it. To the rest of the world you may hear about cancer and treatments and side effects in varying degrees but you are far enough removed it isn’t something you have to think about and experience all day everyday. So the impression you can get of what it’s like is convoluted. Most people just want to focus on the positives. It is treatable. Treatments have come so far. It is curable. They know someone who beat it. I will pray for healing. I know this is how many think because this was me before I had cancer. All of this is wonderful, positive, wishful and hopeful thinking. But for the person going through it and those loved ones walking through it with them, it is a whole different experience even when it’s curable. Being curable really means it can return. Even if being a “survivor” only means a survivor for now and maybe you won’t die from it but the thought of it returning may never go away, but yet you survive. So this blog post is to tell of my experience, for those who really want to learn what it is like through my eyes. Also, for those who really want to know “how I’m doing?” Please know that it is different for everybody. This is my story. These are my details. This is my reality. This post is a lengthy one. Some details are not fun details and very personal. You’ve been warned.
How am I doing? That is the question I get the most on the day after my chemo infusions. It is really a loaded question though. The day after chemo is usually a really good day with minimal side effects. So it does not give anyone asking a good representation of what going through chemo is like for me. When my answer is almost always, “good, just a little tired.” Other answers I usually give throughout my cycle: “I’m doing good,” really means life is tolerable and I’m having an ok day. “I’m ok,” really means life kinda sucks but I’m trying to stay positive. “Not good,” means life sucks bad today and staying positive is really hard.
So, with experiencing chemo #4 today, I want to talk about how I’m doing and what it’s been like for me. I say, what it is like for me, because it is different for everyone. Not only does it depend on how the individual person handles the side effects of chemo but also what chemo meds and other meds the individual is on and the dosages and regimen. It is individualized to each person, their type of cancer, their type of tumor of that cancer, the stage of that tumor, and several other individual factors that effect treatment.
Cancer is not just cancer. Breast cancer is not all the same. Treatment is different for everyone. And chemo is just a piece of the puzzle in the treatment plan and very individualized.
For example for my type of cancer, tumor, stage and age. There where two different and very specific chemo regimens that my oncologist had to choose from that would be the best course of action for me. Those two are specific to just my type of tumor. (HER2 +, ER and PR -). The one that we didn’t go with was not as harsh because it only had 2 meds (1 chemo drug and 1 targeted therapy drug) that would be infused weekly for 12 weeks. The med combination that my oncologist decided was the best for MY specific circumstances was the second option. My chemo regimen is 4 meds (2 chemo drugs and 2 targeted therapy drugs), infused every 3 weeks or 21 days for 6 total infusions, lasting a total of 18 weeks. Referred to as the “big guns.” Because of my age and higher risk of spread and reoccurrence the “big guns” were felt to be necessary. Many people think it is just the chemo meds that are “poison” and come with horrendous side effects. Well all 4 meds come with their own set of harsh side effects.
Let me first share what my chemo day is like. I want to start with my wonderful husband who accompanies me to every chemo day and is committed to being there throughout my treatment for everything, especially the treatment days, Doctor appointments and any other day that is crucial to my treatment, procedures and planning. He has been my rock and has sacrificed so much since the day we found out. He has taken up the role of caregiver selflessly and compassionately. He sees to my every need while coping with his own emotions and fears. All of this while working 50+ hour weeks and taking care of our family. On chemo day he is with me the whole time, he drives me there and sits with me throughout, sometimes just watching me sleep for hours, then drives me home.
City of Hope is in Duarte, Ca. This is where my team of Doctors and specialists collaborate on my care and all my appointments and care is given. It will also be where I have my surgery in March. It’s about 40 min from our home, sometimes up to 60 min in traffic. When we arrive we report to the VAD lab. VAD stands for Vascular Access Device. This is a special department of the lab, staffed with nurses instead of phlebotomists, who can access central lines. I have a port cath placed under my skin below my right clavicle and runs up into my external jugular vein. It is a centrally placed line used for all infusions and lab draws and must be accessed under sterile technique and have a needle placed in it and secured for infusions. In general the port itself and line can easily be felt under my skin and also seen. The port site is a lump about the size of a nickel in my chest. I have two scars from the placement of the port. One over the port itself about an inch long and one tiny one about 1/2cm over the site in the base of my neck just below where the catheter enters my jugular vein. I use lidocaine cream over the port prior to my appointment. Sometimes it works, sometimes it doesn’t. It takes 30min to an hour to be effective, so if it has to be accessed quickly or unexpectedly there is not time for lidocaine cream. That was the case when I had my fainting spell 3 weeks ago and was taken to urgent care at COH. The poke of the IV/infusion needle itself hurts and feels uncomfortable for a period of time after insertion. Often the lidocaine doesn’t work to completely numb the skin and with the exception of one time, it has been uncomfortable with each access.
Once accessed they draw several tubes of blood to run labs that are essential tests to run prior to each chemo infusion to make sure that my body has recovered adequately enough from the last chemo effects and to check my liver function, my electrolytes and my blood count and differential. After drawing labs they secure the needle in my port for use later with chemo, then flush it with heparin to keep the port from clotting.
After my VAD lab appointment, I report to the Women’s Center where I wait, usually about an hour, while my labs are being processed, then I see my medical oncologist for an update. She reviews my labs, my symptoms, my meds and any changes to my plan and treatment, she reviews updates on any test results and specialist consultations and addresses any needs or questions I have. Sometimes this leads to additional scheduling after the appointment for further imaging or consults. One problem or side effect that has revealed itself through my lab work is that chemo is killing off my rbc’s. So in 2 months my hemoglobin has dropped from 14.5 to 9.9, which means I am anemic, which contributes to fatigue, dark circles under my eyes and fainting spells. If it drops to 8 they will have to transfuse. We will see what happens.
After my Doctor appointment I report to the infusion floor to check in for chemo. When I learned that the chemo meds I would be on have a 100% side effect of hair loss but there is a therapy called dignicap or cold cap therapy that has a 67% effectiveness rate, I was interested. It is not covered by insurance and it is not cheap. It is $350 for each session. My chemo consists of 6 separate sessions. My generous and wonderful husband told me from the beginning if it was important to me than we would find a way to pay for it. (I told you he is pretty great!) Hair loss is very personal and everyone feels differently about it and copes with it differently. For me it was a matter of not wanting to “look” like a cancer patient and get that pity look from everyone I encounter. I don’t want strangers to know I’m a cancer patient. I also want to look like myself when I look in the mirror and don’t want to avoid pictures because of it. For me, keeping my hair would be a way I could still feel somewhat normal in a very not normal struggle and year of my life. And yes, hair grows back, but it takes years for hair to grow back out to a pre-cancer length, so that means living with a very outward appearance reminder long after chemo is over. Scars can be hidden under clothes. Lack of hair cannot, except with wigs, which to me are almost just as obvious as scarves, wraps and hats to those who know me and most importantly to me. Also, when you go to bed at night it is usually not with any head covers. My wonderful husband says it wouldn’t bother him, but it sure would bother me. Fortunately I have proven to be in the 67% that cold cap therapy works on. I would have lost all of my hair by the second chemo treatment if I was going to. Although you can loose up to 50% of your hair and still be considered in the 67% group. My hair is thinning but it isn’t noticeable at this point. I try to wash it no more than 2 times a week because I loose the most hair when I wash it and brush it, especially when it’s wet. I could still possibly loose my eyebrows and eyelashes although I haven’t yet, they are not protected by the cold cap.
One benefit to cold cap therapy beside the preservation of my hair is that it means I get a private room during my chemo infusion. I have to be attached to the dignicap machine the entire time of the infusion which lasts about 6 hours, so they put a commode next to my infusion/lounge chair which is the primary reason for the private room. But it is nice having the privacy, the cap looks funny on me. It also gives me a quieter environment to preferably sleep as much as I can through the miserable therapy session and gives my husband privacy being the introvert he is.
The worst part of the infusion experience is the cold cap therapy. You may wonder why I would subject myself to torture that is elective. Again, it’s because keeping my hair is worth it to me and they sedate me pretty heavily to be able to tolerate the pain and discomfort of the most intense brain freeze you can imagine, which is why I am able to sleep for periods of time. If you can imagine what it feels like to stick your entire scalp, wet, in a snow bank, with nothing protecting your head and then staying there for 6 hours, that is the best sensation I can imagine comparing it to.
My infusion session starts with a specially trained dignicap technician securing the cold cap on my head which starts with her saturating my hair with a spray bottle then placing three layers, a thin cotton cap, a rubber type cap fitted to my scalp and then the attachment layer to the machine that locks the cap down to my scalp and wraps it around my chin. They turn two knobs on the sides of my head that lock it down tightly. Once they turn the machine on it is immediate extremely cold water that constantly circulates through the cap and gives me an instant intense painful headache and overall discomfort. It is absolutely miserable initially but with the sedation it gets better and eventually more tolerable as I get used to it. For the first 30 minutes the chemo nurse that is assigned to me loads multiple medications through my IV port, including Ativan sedation, Benadryl, steroids, anti-emetics, acid reducer and any other medications the Dr decides I need based on my labs. I usually also take Tylenol to help with the cold cap headache as well. It takes the full 30 minutes for the cold cap to gradually reach the temperature it has to be at for the chemotherapy infusion to begin.
Once the temperature in the cap reaches 34 degrees then the nurse starts my first of 4 infusions, they begin the chemo medications first over 1-2 hours for each, separately. After the two chemo drugs have infused, the other two targeted therapy medications are infused separately over 1-2 hours each. Once all four medications have infused, the cold cap is turned off and removed. A medication infusion patch called Neulasta is applied to my abdomen before I leave. It injects a needle into my abdomen after applied and stays adhered on my abdomen with a tiny plastic cannula in my subcutaneous tissue until it infuses the medication 27 hours later over a 45 min time period, it then alarms and I remove it. It is a bone marrow stimulant that can help the body make white blood cells after receiving cancer medications.
After all of this, we go home. Once the cap is off, I feel pretty good, just tired. I continue taking oral steroids through the end of the next day. I usually feel pretty good through the next day and into the 3rd day before the steroids wear off and the worst side effects really start kicking in. Fatigue is always present in varying degrees and never completely goes away. Chemo brain kicks in right away, which is a lack of focus and concentration, brain fog, inattentiveness and restlessness. There are other side effects that can happen and don’t go away until after all chemo is complete and some can last for 8-12 months after chemo. Some side effects can even cause permanent issues. Side effects I am unfortunately experiencing that fit in that category are my monthly periods, they have stopped and because of my age, may or may not come back. This is accompanied with menopausal symptoms including hot flashes, so that’s not fun. Secondly, and more serious, I am also experiencing neuropathy symptoms in my hands and feet since after my second infusion, worsening after my third and it is expected to progressively get worse. It often doesn’t go away until months and sometimes years after chemo. There are cases where it is permanent. 30-40% of chemo recipients are effected by varying degrees of neuropathy. For me it feels like a pins and needles sensation in the bottoms of my feet and finger tips and mild numbness and tingling in my feet and hands. This comes and goes throughout the day and seems to be worse when I’m inactive or laying in bed. But it does not go away throughout my 3 week cycles and seems to be worsening, as warned, with each progressive infusion. Fatigue and energy depletion also gets worse with each progressive infusion.
Then there are the side effects that start to kick in on day 3 and last for varying lengths of time. The worst of these and the most annoying is bowel issues, primarily diarrhea accompanied with abdominal cramping. That usually starts by day 4-5 and lasts daily till about day 12-14 and causes the soreness that you would expect especially with all my mucous membranes being raw. That is also a side effect. All my mucous membranes are effected, by day 3 and lasting into the 3rd week in varying ways and cause a variety of issues. Those include mouth rawness, which feels like the entire inside of my mouth, throat and tongue is burnt and raw, this causes problems with nausea, bleeding gums, occasional mouth sores and loss of appetite, also it makes food taste differently and makes it harder to want to eat and drink on the worst of those days. Throat sensitivity and hoarseness occur with overuse of my voice, the rawness in my esophagus causes heartburn that lasts throughout the cycle. Nose rawness leads to dryness which leads to my nose running incessantly by week two and my nose bleeding for several days, up to a week, especially in the morning. My eyes water constantly by week two which drain through my tear ducts and cause my nose to run even more. Other annoying mucous membranes that are effected and not pleasant to talk about, cause vaginal dryness and rawness and rectal rawness.
Day 3-6 I have body aches, nerve pain, tenderness and sensitivity to touch all over, I also have facial flushing, and my scalp and face feel tender to the touch. After my first treatment, I broke out badly with acne all over my face, neck and scalp and was treated with antibiotics. Since then I have been faithfully using an activated charcoal bar from Beauty Counter to wash my face, neck, chest and behind my ears and that seems to be helping a lot with the breakouts. I use moisturizer to treat my dry skin and essential oils for my nails which are dry and brittle. I also use oils for skin breakouts and other breakdown, scars and abrasions. Lip balm is always on my lips to prevent chapping.
By day 4-5 I want to crawl out of my skin, I just don’t feel normal, it is like I can feel my cells dying. It is a miserable sensation throughout my body and this is when it is the worst. My hands and feet get really warm from the neuropathy, nerve and body pain on these days especially. I experience sensations at times of my ears ringing and buzzing and my pulse beating loudly in my ears. I have only had one actual mouth sore so far. But I am really careful with oral care and I rinse with biotene and salt water/baking soda mixtures because of the rawness and burnt sensation. I brush with a special, extra soft bristle tooth brush. This helps with the rawness and bleeding. I get completely depleted doing simple things like taking a shower or climbing the stairs. I stay in bed a lot or lay on the couch most of the day. I have difficulty sleeping some nights or wake up frequently.
Day 4-6 is the worst of the symptoms and they are pretty constant. Day 7-14 I may have several good hours (good means ok in comparison) and then several bad hours lasting different lengths and times of the day. I never know when the worst of it is going to hit. So I stay close to home mostly. Day 14-21 get better, some symptoms have gone away, my energy level increases and I feel pretty good for most of the week before my next infusion. During this time the lingering issues are mostly annoying but tolerable, usually lessening of the fatigue, watery eyes and runny nose and occasional queasiness. I have only thrown up once.
This last cycle I got sick with a cold prior to chemo and it settled in my chest and even though it never got very serious, the phlegm and productive cough and on and off throat irritation lasted for over 3 weeks. It is very hard for my body to heal and very easy to catch infections and viruses because my entire immune system is suppressed and my white count depletes. The typical days when research shows white count dips lowest is days 7-12. Then it begins to recover to normal in time for the next chemo infusion. The Neulasta injection is supposed to help boost white cell production in the bone marrow which can cause bone pain. I take Claritin to help prevent this histamine response. I also have multiple PRN (as needed) medications for some of my symptoms, including antiemetic/nausea meds, an antidiarrheal, antacids, lidocaine rinses, anti-anxiety medication, pain meds, allergy meds, throat spray, and other topical OTC creams and ointments. I pretty much keep a pharmacy with me.
My tastes have changed and change on and off throughout the 3 week cycles. Some days what I can eat or what I have an appetite for is limited. I have to force myself to drink anything because of the rawness and queasy sensation in my throat. Sadly I have lost my enjoyment of the flavor of coffee by day 3 and don’t get it back until about day 16 or so. So I have learned some flavored teas that I like. I cannot drink green tea because it actually counteracts the chemotherapy.
This is my new normal for now. So when you ask me how I’m doing on day 2 or 3, or day 16 or 18 or 20. I may tell you I’m feeling pretty good. Because in comparison, I am. But this is my life for 21 solid weeks including the 3 weeks of side effects following the last chemo infusion. Then I will continue the infusions of 1 of the targeted therapy medications (not a chemo drug). It is called Herceptin and I will continue to receive this infusion every 3 weeks for an entire year, with follow up echocardiograms and cardiologist consults every 3 months for the duration of treatment because of possible adverse side effects of this medication. Most of my side effects will stop and the lasting ones should go away during this time.
After the #6 and final chemo infusion, 4 weeks later on March 12th, 8 days after my 30th wedding anniversary, I will have an incredibly intense and hard surgery that takes 3 months to recover from. The surgery is 12-14 hours long, 4-5 days in the hospital and 3-4 weeks with drains in. I’ve been told I will walk hunched over like a granny for nearly a month and will have weekly Doctor appointments and OT/PT follow up.
The good news, chemo works! After my first infusion prior to my second, I could tell the tumor had shrunk considerably. After my second infusion, I could no longer feel it nor could my doctor. After my third infusion I had a follow up breast ultrasound and it showed that it was less than half the size of what it was when I started chemo. At the halfway mark Chemo has shrunk more than half the tumor. So we know that even though the treatment is awful, and harsh to the body, it does it’s job very effectively!
Most people don’t ask how my husband is doing which is something he notices. When we go anywhere and see people everyone asks how I’m doing and gives me attention and shows concern over me but almost never ask him. He says he doesn’t mind really because he doesn’t like the attention or having to answer questions anyhow but he says he can see how it could really bother people with different personality types. He is amazing. He is such a source of strength, compassion, understanding, service, care and stability. He works 10-11 hour days and comes home wanting to serve me. He caters to all my needs and tells me constantly, you should be resting. He checks in on me throughout the day and I know if I told him I needed him home he would come immediately. He is walking through this with me, literally. I can describe to all of you what this is like for me but he actually experiences it all with me. It becomes a lot more real and difficult to watch a loved one experience when you are physically there watching them go through it. When you come home at the end of an already heavily stressful day and ask how their day went and you get all the details. When you check in throughout the day and hear the updates and wish desperately you can be there with them so they don’t have to be alone while they suffer. Then there is the fear and the unknowns of being married to and wanting to grow old with your best friend and love of your life and not knowing what the future holds for them. He has to hold it together everyday for me while I’m given permission from everyone to fall apart as needed. This is his experience. This is his new normal.
I wrote this post to focus more on the chemo experience and treatment plan for me and what my future treatment plan will entail. To help others who would like to understand my experience and truly know how I’m doing. I could write so much more about the mental, emotional, and spiritual aspect of my journey. But I will save that for another day. God has been so faithful and so present. I walk through the valley of the shadow with Him right there with me. His will, not mine. His plan is perfect, and I am content in his peace as I walk with him in his plan for me to bring glory to His Name.
There is hope beyond this!
So well written Rebecca. You are an awesome writer and your skills are blessing others. The details of what you both are enduring has helped me understand what my sister, sister-in-law, best friend and others have gone through. My heart and prayers are with you and Danny and your family as you face and conquer this battle. It’s hard, but you are already victorious. I’m so very proud of you both. Love to you and thank you for sharing.
LikeLiked by 1 person
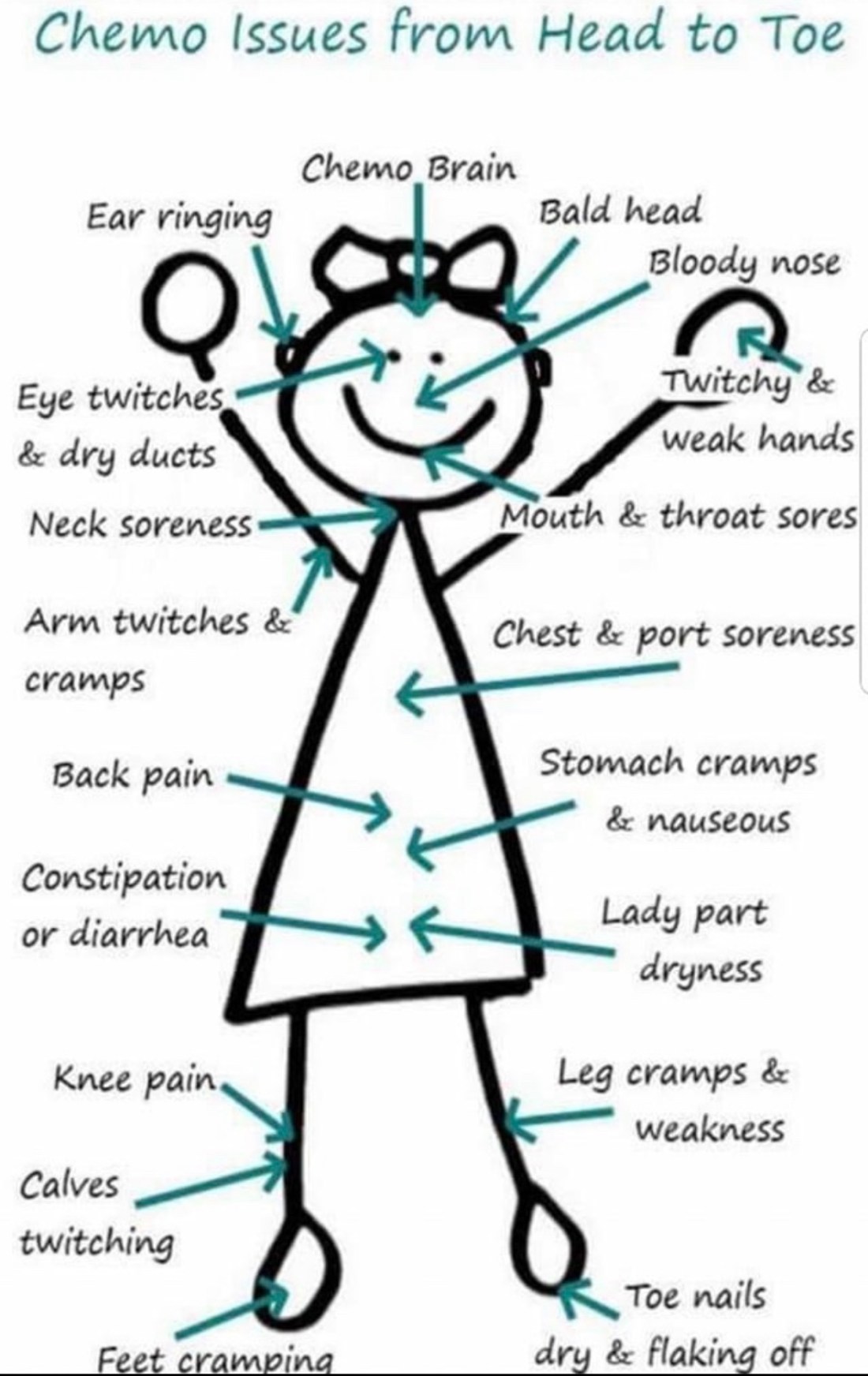
Hi Rebecca, I a wanting to use the graphic ‘Chemo Issues from Head to Toe’ in my Breast Cancer book. Is this your work? If not, can you tell me the source. I’d like to reference and acknowledge it.
LikeLiked by 1 person
Honestly I don’t remember. I’m sure I saved the photo off some post on FB, but I don’t know the source. Sorry 😣
LikeLike